President’s Message
“Nothing travels faster than the speed of light, with the possible exception of bad news, which obeys its own special laws.”
Summary: A personal account highlights the shift from delivering “bad news” to “unexpected news” in healthcare to foster hope and reduce traumatic patient memories, emphasizing that empathetic, patient-centered care is as critical as technical expertise. The author, diagnosed with Merkel Cell Carcinoma, underscores the importance of interdisciplinary care and cultivating an institutional culture that treats the human, not just the disease.
Steve receiving Radiation Therapy
As health care professionals, we often have to deliver “bad news” to our patients, although the term “unexpected news” is currently being used as a proactive replacement or an alternative phrase to “bad news.” This change reflects a move toward reducing provider bias, fostering hope, and adopting a more family-centered approach. Another significant reason why this shift is happening is to reduce the “flashbulb” memory of the patient; the initial words that were used are remembered for a lifetime, triggering unpleasant memories.
Every profession, specialty, or subspecialty has its own unique circumstances that may require providers to give their patients unexpected news. The specialists who deliver the most “unexpected news” are the oncologists. They diagnose cancer and discuss disease progression, or a terminal prognosis, with an average of 35 patients a month. Emergency physicians deal with sudden, unexpected trauma and death. They often have to break devastating news to families with whom they have no prior experience or relationship, under extremely stressful situations. Obstetricians and gynecologists often have to confront patients with “unexpected news” related to infertility, miscarriages, fetal abnormalities, and high-risk surgical complications.
Thinking of what my president’s message would be this month, I had a recent experience that I would like to share with our HELEN readers.
In two months, I will be 80 years old, have unlimited energy, exercise regularly, will be celebrating my 58th wedding anniversary, and have children and grandchildren who live close by and whom I see regularly. I am blessed to be in a great space, love my family, friends, and everyone involved in my life.
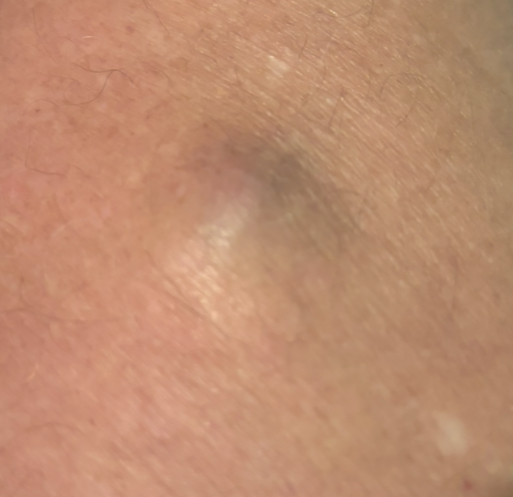
Over a year ago, I noticed a small mass on the anterior aspect of my right thigh, midway between my knee and groin. It was painless, initial growth was slow over several months, and it remained stagnant, only changing slightly in appearance to a slight bluish color. I showed it to multiple physician colleagues over the year, and everyone diagnosed it as a cyst or lipoma, but only on visualization.
Recently, having a routine health checkup, I decided to consult with a plastic surgeon friend of mine to just take a look at the lesion and evaluate it. The following day, I saw him, and he excised it and sent it to the lab for testing. Healing was normal except for a hematoma, or bruise, because I take a blood thinner twice a day.
Twelve days later, I went for my suture removal. Upon entering the room, my friend asked me if I had seen the lab report on the patient gateway. I replied I hadn’t, and he said, “Good.” He then proceeded to tell me he had “bad news” for me.
“What do you mean, bad news?” I asked. “It was nothing, a lesion on my thigh. What could possibly be bad news about it?”
He said, “No, it’s really bad. You have Merkel cell carcinoma.”
I replied, “WHAT?! Are you serious? What is the five-year survival?”
He hesitantly said maybe less than 50%.
From that point on, I was unable to process anything, only thinking of how I would tell my wife and family. How would I break the “bad” or “unexpected” news to them? In that instant, my life would forever change. My surgeon said he had a colleague at the Dana-Farber Cancer Institute in Boston, immediately contacted him, and within two hours I received a call from a reassuring team coordinator who comforted me and said, “Don’t worry, we got you.”
“The good physician treats the disease; the great physician treats the patient who has the disease.”
Two days later, our family trip to see the surgeon was a cry fest of doom and gloom for my daughters, wife, and myself. We checked into the Cutaneous Cancer Center, and everyone we met was as kind and gracious as they could be. From the minute the surgeon entered the room, he never looked at the computer or cellphone, sat among the four of us, hugged us, held our hands, or did whatever he deemed necessary to assure us that his team would provide me with the latest state-of-the-art care in a positive, empathic, patient-centered, caring environment.
We laughed, we cried, we hugged, and left with a calm, positive attitude, knowing we were in good hands. We immediately felt the clinician’s empathy, his sharing our feelings, putting himself in our shoes, as opposed to sympathy, which is understanding but from another perspective.
Four days later, I had a PET scan and three one-hour consults with the medical, dermatology, and radiation oncologists. The culture of Dana-Farber uplifted us all and put us in a good space. Again, except for reviewing the PET scan, each clinician maintained constant eye contact, positioned themselves in the center of our family, and embraced us when we needed it. It was decided that my treatment would only require radiation therapy.
Two days later, I had a telemedicine consultation with the nurse practitioner to review the scan and the team’s decision to immediately begin radiation five times a week for six weeks.
I am sharing my personal story for several reasons. First, one of our most common expressions in Developmental Medicine is, “If you hear hoofbeats, it is almost always a horse, but occasionally it could be a zebra.” I had the zebra, and early diagnosis and treatment are imperative. If a strange lesion appears on you or your patient’s skin, then please seek a specialist consultation.
My second point is to deliver unexpected news to the patient in the kindest way you can, eliminating any chance they have for their “flashbulb moment.” As an academician for 50 years, I try to instill in every student the quote from Dr. Francis Peabody, which he gave to Harvard students at Boston City Hospital on October 21, 1926. His words were, “The secret of the care of the patient is in caring for the patient.”
Who was Dr. Francis Peabody? He was born into a prominent New England family in 1881 and received his medical training at Harvard and Johns Hopkins. He was known to be an excellent bedside teacher and a clinical investigator. His famous lecture was printed in the Journal of the American Medical Association in 1927, (JAMA; 88:877-882) the year of his death due to cancer, and it is still one of the most revered articles in medical literature.
Another point, as I have begun my five-day-a-week for six weeks radiation therapy, is how the “culture” of the institution is vital to patient care and outcomes. The Dana-Farber Cancer Institute, in particular, the Cutaneous Skin Cancer Treatment Center, signifies to me everything we have fought or wished for our patients from the American Academy of Developmental Medicine and Dentistry (AADMD), People Advocating for Optimal Health (PAOH), HELEN Journal, and all the allied organizations I participate in. An interdisciplinary, comprehensive team approach combining leading experts and the latest advances in technology and research.
Dr. Peabody’s words that “the essence of the practice of medicine is that it is an intensely personal matter” mean that we must not forget we are treating a human and not a disease process. Hospital experiences are often dehumanizing, not recognizing the patient who is surrounded by their home, work, relations, friends, joys, sorrows, hopes, and fears.
I can’t even begin to thank enough the countless people I encounter every day I walk into Dana-Farber for their creating of the most ideal “Medical Home” anyone can ever experience.
About the Author
Steve Perlman, DDS, MScD, DHL (hon) President, People Advocating for Optimal Health (PAOH) Special Projects Sr., Editor Helen: The Journal of Human Exceptionality