Special Care Dentistry in Africa
A conversation with Dr. Cathy Makobe-Chiloane on expanding access to oral healthcare for people with disabilities in South Africa.
By Helen Journal Staff
Summary: South African dentist and educator Dr. Cathy Makobe-Chiloane discusses the challenges of providing dental care for people with special healthcare needs, the lack of formal Special Care Dentistry training in many dental programs, and the importance of advocacy, education, and compassionate care. Drawing on her clinical experience, teaching, and community outreach, she shares strategies for treating patients with disabilities and encourages dentists worldwide to make their practices more inclusive.
There’s clearly a need for more oral healthcare professionals such as you, to make a deliberate attempt to welcome more people with disabilities into their clinics. Please share your thoughts on that. Are dentists in your country required to treat all patients who come to the clinic, or can one turn them away if there’s a discomfort regarding treating people with special needs? Do many get turned away?
“In South Africa, Paediatric Dentistry is not recognised as a formal specialty, and Special Care Dentistry (SCD) is largely absent from undergraduate and post graduate curricula—except at my university, where I introduced SCD in 2018. Since then, final-year dental students receive lectures in SCD and are allocated one clinical session in the SCD Unit. While we have a few dentists with a special interest in Paediatric Dentistry and SCD, general dental practitioners are expected to treat all patients presenting at public and private facilities.
Unfortunately, some clinicians choose not to treat paediatric patients or patients with Special Healthcare Needs (SHCN), across all age groups, which is a big challenge in our country. As a result, these patients are often turned away or referred to Academic Dental Institutions for treatment—a phenomenon sometimes referred to as “passing on the responsibility.” Academic institutions, therefore, must find ways to accommodate and treat these patients. Most of these patients present as emergencies and often require extensive treatment under general anaesthesia (GA).
In South Africa, out of the nine Provinces- Gauteng Province, has three academic dental institutions, which are among only five such institutions in the entire country; one of the five institutions offers training in Oral Hygiene and Dental Therapy only. Similar to Paediatric Dentistry, only a few dentists have a specific interest in treating patients with SHCN, whether in the public or private sector. Treatment under GA remains the most common modality. Unfortunately, in private practice, GA is largely limited to patients who are financially privileged.
Of the three academic institutions, my institution has historically been the most stable in providing dental treatment under general anaesthesia (DTGA) until November 2024, when our anaesthetist resigned. Since then, DTGA services for SHCN patients have been suspended. A sessional anaesthetist was appointed in July 2025; however, services for SHCN patients have not yet been fully reinstated. Currently, SHCN patients who require extractions but are uncooperative in the dental chair are referred to a sister hospital, which only performs extractions under GA. The sister hospital does not have dental equipment in theatre to provide comprehensive dental treatment under GA.”
Where did you go to dental school? What did they teach dental students regarding how to treat people with special needs?
“I completed my undergraduate dental training at Medunsa, now known as Sefako Makgatho Health Sciences University. It is the only medical academic health institution in South Africa that was historically established, prior to 1994, to serve previously disadvantaged populations—specifically Black South Africans.
I qualified in 2000 as a General Dental Practitioner/Dental Surgeon (BDS). I completed my community service year at Mokopane Hospital in the Limpopo Province, after which I was retained by the same institution. I later moved into private practice while continuing to work part-time at the hospital, eventually returning to full-time service approximately four years later. South Africa has nine provinces, and Limpopo is recognised as one of the poorest. During my undergraduate training, Special Care Dentistry was not included in the curriculum—an unfortunate gap that persists to this day.
From early on, I was particularly passionate about Paediatric Dentistry, Preventive Dentistry, and community outreach. This commitment was shaped by the numerous challenges and barriers that Black communities continue to face in accessing healthcare services, especially oral healthcare. Within the broader healthcare landscape, and more specifically within Paediatric Dentistry, I recognised that my role would always be essential. Children will always be born, and they remain cherished by their families—their “bundles of joy”—regardless of whether one works in the public sector or private practice.
Limpopo Province embraced me warmly, and I remain deeply appreciative of my experiences there. Working in this environment taught me invaluable lessons: professionalism, punctuality, teamwork, and the ability to work effectively with individuals across a spectrum of roles—clinical staff, support staff, cleaners, security personnel, and administrators. As the first person in my family to attain this level of education and professional responsibility, I had no familial guidance to rely on. This made the journey both challenging and profoundly meaningful.
In 2006, I joined the University of Pretoria Oral Health Centre as a joint appointee, working for both Gauteng Health (public sector) and the University of Pretoria as a lecturer.
I initiated the Eastern Cape MEC Oral Health Outreach Program in 2019, which is supported and funded by the Department of Education (DOE). This program is an annual, week-long initiative focused on oral health awareness, education, and promotion in special schools across the province.
Eastern Cape Oral Health Outreach Program
The program is conducted in collaboration with a multidisciplinary team of health professionals who assess learners for appropriate school placement. These include occupational therapists, audiologists, speech therapists, social workers, psychologists, optometrists, and others.
Our dental team provides dental screenings and emergency treatment to learners, their parents, and teachers. Each participant receives a goodie bag containing a toothbrush, toothpaste, dental floss, and educational pamphlets. The program primarily targets rural areas that are far from health services. The DOE supports logistics by providing transport for parents and learners as well as healthy meals during the program.
The oral healthcare professionals who participate in the week-long program volunteer their time. Some are early-career professionals seeking exposure and experience in managing patients with special healthcare needs (SHCN). The DOE covers flights, transport, and accommodation for all participating health professionals and NGOs.
This program has provided a comprehensive, multidisciplinary approach to oral health promotion, while improving access to essential dental care for underserved and vulnerable populations in the Eastern Cape Province.”
How many years have you been in practice, and what was it like with your first dental patient with a disability?
“I have 25 years of experience in Dentistry, including 20 years dedicated to Paediatric Dentistry and Special Care Dentistry. After working in the public sector for several years, I transitioned into academia, where my passion for serving children and individuals with special healthcare needs (SHCN) continued to grow.
I cannot clearly recall my very first patient with SHCN, largely because patients with special needs were consistently included on my theatre lists due to the limited access to operating theatre time. I spent a great deal of time engaging with parents—listening to their stories, trying to understand their challenges, and learning how they were coping. This was long before I had my son, Thapelo, and I did not realise at the time that these interactions were quietly preparing me for a personal journey ahead.
Advocating for patients with SHCN came naturally to me. I fought for them to receive the best possible care, to be prioritised appropriately, and to have a voice in a healthcare system where they were often overlooked. This advocacy was not always welcomed by colleagues, particularly given the long theatre waiting lists for paediatric cases, but I persisted because I understood the urgency and the need.
Thapelo was born on 11 December 2009, and I discovered his condition at birth. Initially, I felt uncertain and overwhelmed. However, after returning from maternity leave, my commitment to treating patients with SHCN intensified—now strengthened by my personal experience and profound empathy. My lived experience as a mother became a lifelong source of insight. I transformed my pain into power and purpose.
I began advocating more intentionally for equitable access to healthcare—especially oral healthcare—for individuals with disabilities. This required extensive reading on policies, legislation, and broader issues such as access to appropriate therapy, inclusive education, social support, and disability grants. I read extensively—books, articles, and professional resources—and watched numerous videos to deepen my understanding of Special Care Dentistry. Although much of my learning was self-taught, my greatest teacher was my son. It was through this journey that I was eventually introduced to Special Olympics.
My involvement with Special Olympics began in 2012, the same year I trained as a Clinical Director. Around that time, I was also introduced to Dr. Steve Perlman—the founder of Special Olympics Special Smiles—who was described to me as a visionary and a true force in the field. I was often told that I had to meet him someday.
That opportunity finally came in 2017 when I travelled to Graz, Austria, for further training as the Regional Clinical Advisor for Africa. Meeting Steve was an unforgettable moment; he was incredibly excited to meet me, and I was absolutely over the moon. I also met several distinguished clinicians, including Dr. Allen Wong and his wife Karen. The love, warmth, and unwavering support I received from them, along with the depth of knowledge they shared, have stayed with me to this day.
I continue to be actively involved in Special Olympics initiatives. In 2018, I attended the 24th Congress of the International Association for Disability and Oral Health (IADH) in Dubai. The support and encouragement from Steve and Allen have only continued to grow—fuelling my passion, strengthening my commitment, and keeping me inspired and hungry for more.
I also joined the Tshwane Down Syndrome Association and later served as a board member, in addition to contributing to other NGOs supporting persons with disabilities. In 2014, I received an award recognising my work as both a mother and a dental professional advocating for oral health. In 2016, I was nominated to serve on the Presidential Working Group on Disability (PWGD) in South Africa—a role I continue to fulfil, with 2025 marking my final year of service.”
Describe in detail your experiences as a dentist and lecturer at the University of Pretoria (or wherever you’re currently working) specifically when it comes to treating people with disabilities. (Have you practiced, at any time, in America? Any comments would be welcome about your thoughts regarding this experience.)
“I have never worked in America, let alone being in the US.”
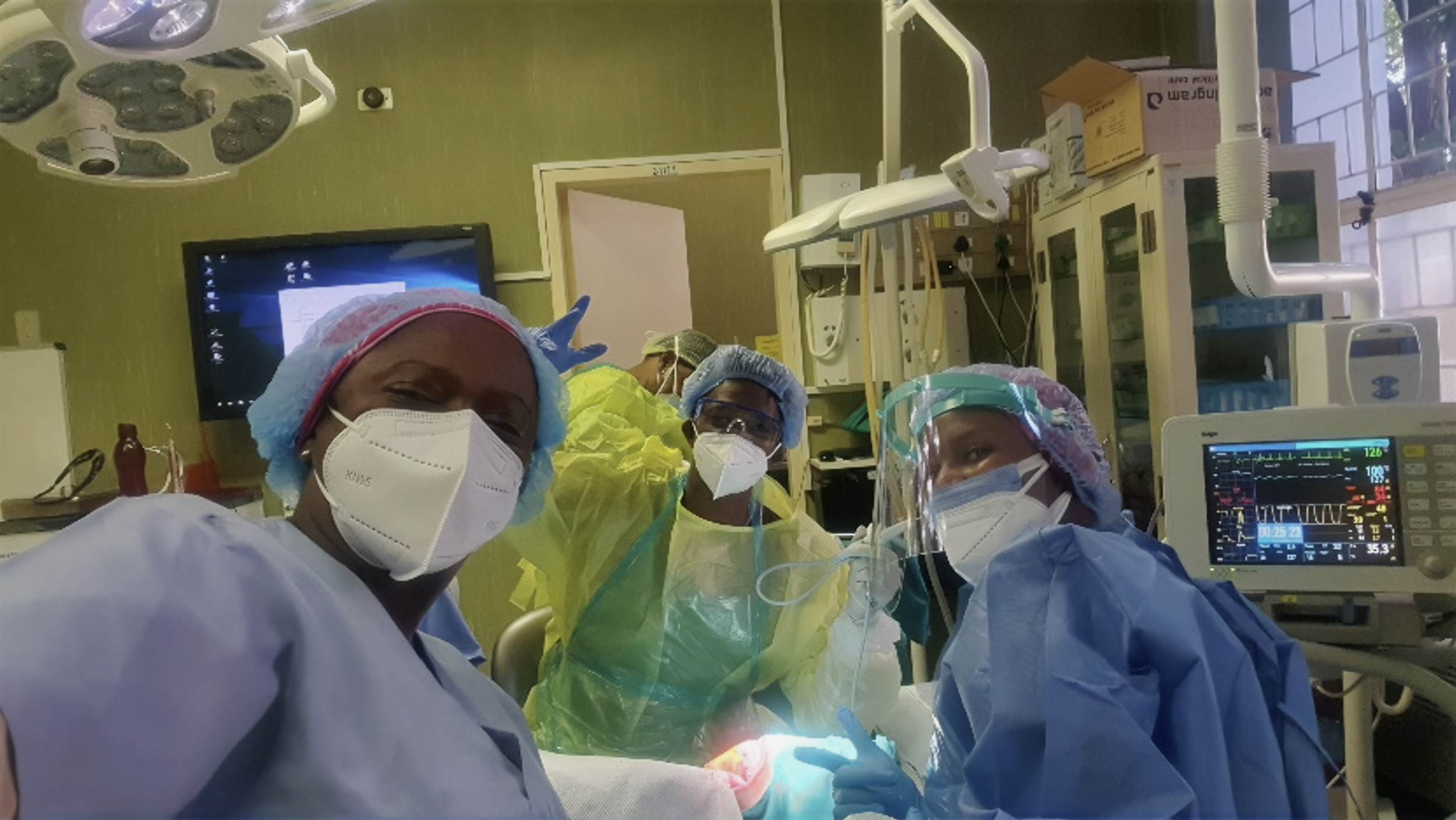
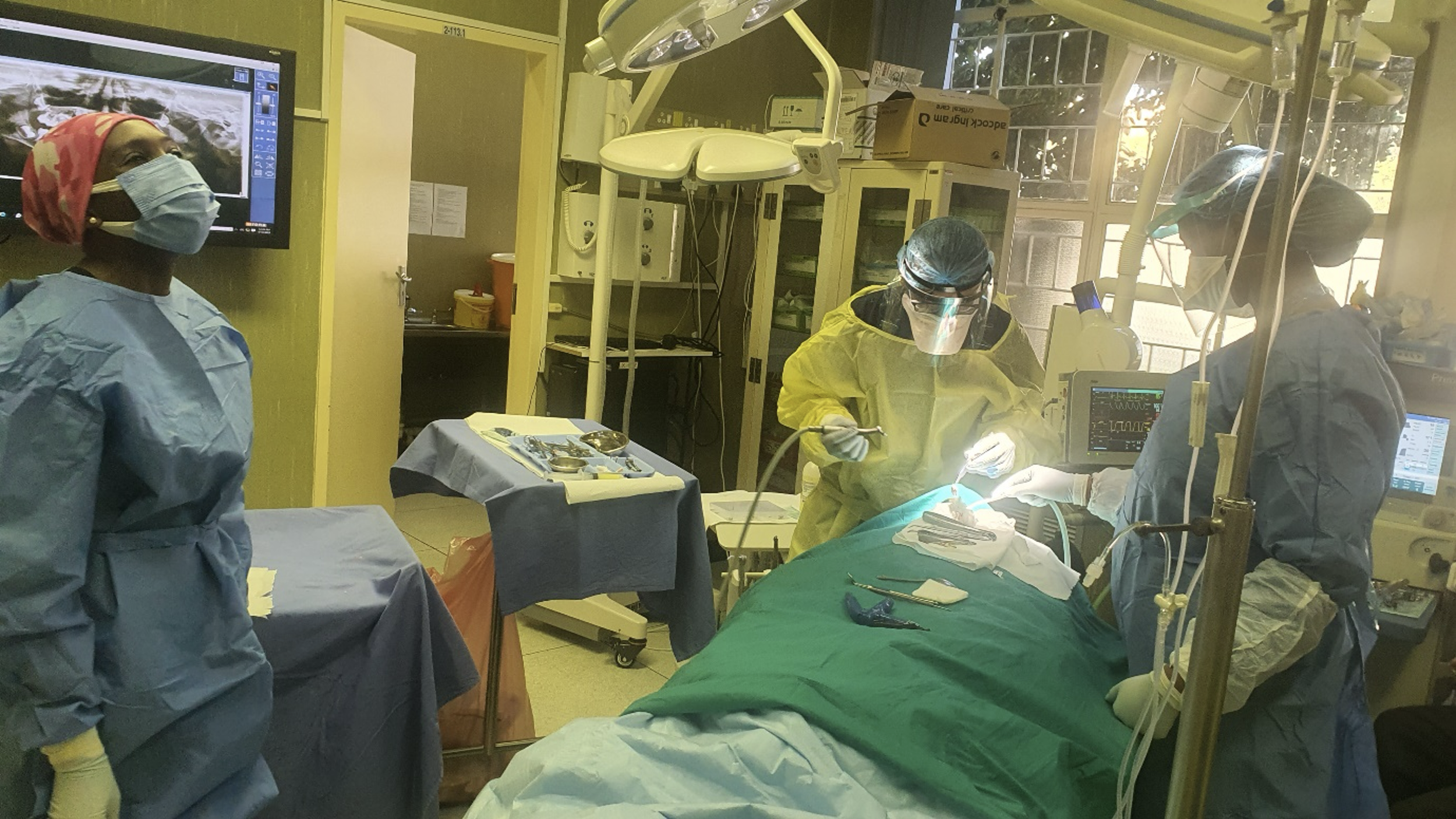
Dr. Makobe-Chiloane in theatre.
What kinds of disabilities do some of your patients have? Just maybe two examples, and how do you prepare for treating them? For instance, if a child has autism and may be sensitive about being touched, which is really prevalent, how do you prepare for that?
“The type of disabilities, from the most common ones such as Down syndrome, Autism Spectrum Disorder, Cerebral Palsy, Deaf, Blind, Hydrocephaly, Albinism, Epilepsy, Intellectual Disability (ID/IDD) and so forth, to the most rare ones such as Noonan syndrome, Progeria, CHARGE syndrome, Duchenne muscular dystrophy, Dandy-Walker syndrome, Fibrodysplasia Ossificans Progressiva (FOP), Subacute Sclerosing Panencephalitis, Lennox-Gastaut syndrome and so forth.
Treating autistic patients—particularly those who are sensory-sensitive, anxious, or overwhelmed by touch—requires thoughtful preparation, planning, and environmental adjustment. The goal is to create a predictable, calming, low-stimulus experience that respects the patient's sensory needs while ensuring safe and effective care. Whenever possible, we send parents a “Get to Know Me” form, which they complete in advance. This allows us to gather important information and prepare for the patient as thoroughly and effectively as possible.
Providing dental care to patients with SHCN requires a unique combination of personal qualities, clinical skills, and specialised approaches. The following characteristics and strategies are essential:
Patience: SHCN patients may need more time for communication, acclimatisation, and treatment. Patience allows the clinician to proceed at the patient’s pace, reducing anxiety and increasing cooperation.
Empathy and Compassion: Understanding the patient’s challenges, limitations, and experiences enables the dentist to deliver respectful, person-centred care.
Flexibility and Adaptability: Each patient presents differently. Clinicians must be willing to adjust treatment plans, appointment lengths, techniques, and expectations accordingly.
Strong Communication Skills: Effective communication with patients, families, and caregivers is essential. This includes using simple language, visual aids, gestures, and alternative communication methods when needed.
Behaviour Management Expertise: Knowledge of non-pharmacological behaviour guidance techniques—tell-show-do, desensitisation, positive reinforcement, visual schedules—is critical.
Teamwork and Collaboration: Working closely with caregivers, therapists, medical professionals, and educators ensures coordinated care and better outcomes.
Clinical Competence in Modified Techniques: The ability to use adaptive equipment (such as positioning aids), provide sedation when appropriate, and recognise when general anaesthesia is required.
Cultural Sensitivity: Recognising and respecting diverse backgrounds, beliefs, and values that may influence care.
Problem-Solving Skills: Clinicians often need creative solutions to accommodate physical limitations, behavioural challenges, or environmental barriers.
Resilience and Emotional Strength: Caring for SHCN patients can be emotionally demanding. Resilience helps maintain high-quality care without burnout.
Respect for Dignity and Autonomy: Ensuring that every patient is treated with dignity and involving them, to the extent possible, in decisions about their care.”
What about treating a person with CP that moves a lot? How do you go about treating them?
“Some patients with cerebral palsy (CP) require treatment under general anaesthesia. For those managed in a conventional dental setting, we use supportive positioning aids—such as bean bags and cushions—to enhance comfort and safety. We also utilise Protective Stabilisation techniques when appropriate, including devices such as the Papoose Board, Rainbow Wraps (full-body immobilisation), and Posey straps for extremities, along with mouth props and other adjuncts.
For all patients with special healthcare needs (SHCN), treatment is first attempted in the dental chair using non-pharmacological behaviour management techniques such distraction, Tell Show Do, Desensitisation, reward etc. If additional support is required, oral sedation—typically Dormicum (midazolam), either alone or combined with Protective Stabilisation—may be used and Inhalation Sedation. If these approaches are unsuccessful or inappropriate, the patient is then managed under dental treatment under general anaesthesia (DTGA).”
How do patients with a disability, or parents who have a child with a disability find out about your dental practice? You must be getting so many requests from these families. If so, how do you keep up? Do you make or get referrals?
“I hold a joint appointment, working for Gauteng Health in the public sector while also serving as a lecturer at the University of Pretoria Oral Health Centre. I train final-year dental students in Special Care Dentistry (SCD), ensuring that by the time they complete their studies, they are familiar with the unit, its purpose, and its patient population.
As a tertiary academic institution, we receive referrals from government clinics, community health centres, and district hospitals across the province. In addition, I am actively involved in the Special Olympics Special Smiles Programme and regularly participate in awareness campaigns at various NGOs supporting persons with disabilities, community outreach initiatives, and special schools.
Through these activities, parents, centres, and care homes become aware of the services we offer, or they are referred to us following screening events. In South Africa, this aligns closely with the objectives of the Integrated School Health Programme (ISHP), which further supports early identification and appropriate referral of children with special healthcare needs.”
What or who encouraged you? What would you say are the personal rewards or sense of fulfilment you derived from treating people with disabilities?
“My son has been the greatest driving force behind my practice in Special Care Dentistry. While I initially chose dentistry as a career and developed a strong interest and passion for Paediatric Dentistry, it was through my experiences as his mother that I was guided further into Special Care Dentistry. He made me acutely aware of the significant gaps that exist in our dental curriculum and inspired me to take action to address them. Although progress has been made, many challenges remain, and there is still much work to be done to ensure these gaps are fully recognised, addressed, and adequately supported.
Throughout my journey in Special Care Dentistry, I have been inspired and encouraged by a remarkable network of friends, mentors, and colleagues—many of whom I would never have met without this path. Among them are Dr. Steve Perlman, Dr. Allen Wong and his wife Karen, Barbie, Imke, and Young Kim, whose guidance, support, and passion have profoundly influenced my professional growth.
I have also been greatly encouraged by the Special Olympics Healthy Athletes Program at the international, African, and South African levels, as well as by the colleagues and peers I have met through participation in both the Winter and Summer Special Olympics Games. Additionally, professional gatherings such as the International Association of Paediatric Dentistry (IAPD) and the International Association for Disability and Oral Health (IADH) have provided invaluable mentorship, knowledge sharing, and inspiration.
These experiences, relationships, and collaborations have not only enriched my practice but have also reinforced my commitment to advocating for equitable oral healthcare for individuals with special healthcare needs.”
What advice would you give other practicing dentists to inspire them to open their doors, like you have, to treat more people with disabilities? What advice would you give dental students and other oral healthcare professionals about treating people with disabilities?
“Treating patients with SHCN is not just dentistry—it’s advocacy, compassion, and impact. To have an advocacy Mindset: Dentists often become the voice for patients who cannot advocate for themselves. This includes fighting for access to care, appropriate referrals, and systemic support.
Treating patients with SHCN is one of the most rewarding paths a dentist can take—both professionally and personally. For practicing dentists, my advice is simple to start small, be patient, and to commit to continuous learning. To see the person, not just the condition, and to use welcoming skills to open doors, create access, and make a real difference in lives that are often overlooked. Even seeing one patient at a time can make a profound difference. Educate yourself, seek mentorship, and embrace flexibility—sometimes the most important tools are empathy, understanding, and a willingness to adapt. Collaborate closely with caregivers, advocate for your patients, and celebrate the impact you create in their lives.
To dental students and other oral healthcare professionals, I would say: see the person, not just the condition. Understand the barriers they face, learn behaviour guidance techniques, gain practical experience, and always treat patients with dignity and respect. Use your voice to promote inclusion and access to oral healthcare. Special Care Dentistry requires lifelong learning, curiosity, and compassion—qualities that will serve you well throughout your career. Opening your doors to patients with special needs is not only about providing care—it is about making a meaningful difference in lives that are often overlooked, advocating for equity, and inspiring change in the profession. Every small step matters.”
Dr. D. Cathy Makobe-Chiloane has a dedicated professional interest and passion in Paediatric and Special Care Dentistry. She earned her Bachelor of Dental Surgery (BDS) degree from the Medical University of Southern Africa (MEDUNSA), now Sefako Makgatho Health Sciences University (SMU), in 2000. She furthered her training at the University of Pretoria, where she obtained a Postgraduate Diploma in Paediatric Dentistry (2008) and a Master of Science in Dentistry (MSc Dent) in 2020. Post Graduate Certificate in Paediatric Dentistry for Patients with Special Health Care Needs: Tech School of Dentistry, UK 2024.
Her academic career includes serving as a Paediatric Dentist and Lecturer at the University of Pretoria (2006–2017). She subsequently joined the Medunsa Oral Health Centre (SMU) in the Paediatric Dentistry–Restorative Dentistry Department (2017–2018). In 2018, she returned to the University of Pretoria Oral Health Centre to establish the Special Care Unit for Oral Health Care Services, dedicated to providing comprehensive care for individuals of all ages with Special Health Care Needs. This unit is the first of its kind across Oral Health Academic Institutions in South Africa.
Beyond her academic and clinical work, Dr. Makobe-Chiloane has been actively involved with Special Olympics South Africa since 2012, serving as a Special Smiles Clinical Director and local volunteer. In 2017, she was appointed Special Olympics Special Smiles Regional Clinical Advisor for Africa (Train-the-Trainer) as well as Special Olympics International Volunteer. Her work reflects her deep commitment to improving access to both general and oral health care for paediatric patients and individuals with Special Health Care Needs across all age groups.
Dr. Makobe-Chiloane is an active member of several professional organisations, including the International Association of Paediatric Dentistry (IAPD), the International Association for Disability and Oral Health (IADH), the South African Association of Paediatric Dentistry (SAAPD), and Special Care Dentistry (SCD). She represents both South Africa and the African continent on the Advisory Committee of the IADH.
In addition, she contributes significantly to community engagement initiatives. She is a member of the South African Presidential Working Group on Disability and actively promotes oral health care awareness, education, and outreach. Her outreach work includes conducting oral health screenings and education programmes across various provinces in South Africa, further demonstrating her strong advocacy for the rights and health of persons and children with Special Health Care Needs.